“My dog needs surgery to remove a tumor in his stomach,” said the voicemail.
His family vet wisely recommended an ultrasound, which revealed a mass about the size of a cherry at the “bottom” of the stomach. It was so large that it prevented the stomach from emptying properly. Statistically, there was a high chance of cancer…
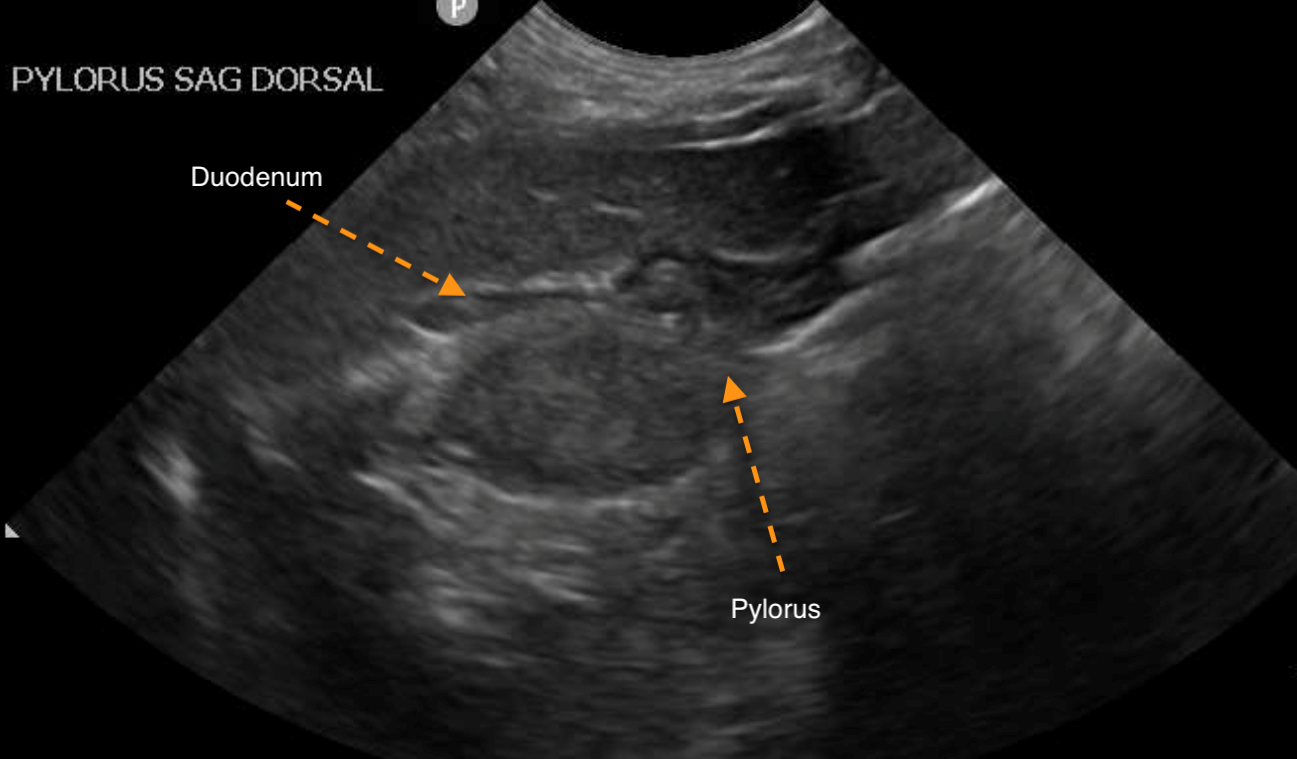
And that is when Max’s owner called me. We went over a few options:
A. removing the mass might be difficult or risky, if not impossible, due to its location.
B. Place a feeding tube to bypass the mass yet provide enough calories to Max.
C. if everything else fails, we could do a “bypass” procedure to allow eating and digesting in spite of the mass.
Option B, which is not for everybody, was rejected. That left us hoping for option A, with option C as a backup plan. The most concerning abnormality on preop blood work was a very low red blood cell count (23%) (the low end of normal is around 35%).
Max’s owner remembers how difficult her decision was: “To what degree he will recover? Is the tumor cancerous? Is this fixable? What kind of quality of life will he have? Are we investing in his life, or are we being selfish by keeping him around if he is going to be in pain?”
Chest X-rays did not show any spreading to the lungs, so we took Max to surgery. We confirmed a mass, about the size of a cherry, at the “bottom” of the stomach.
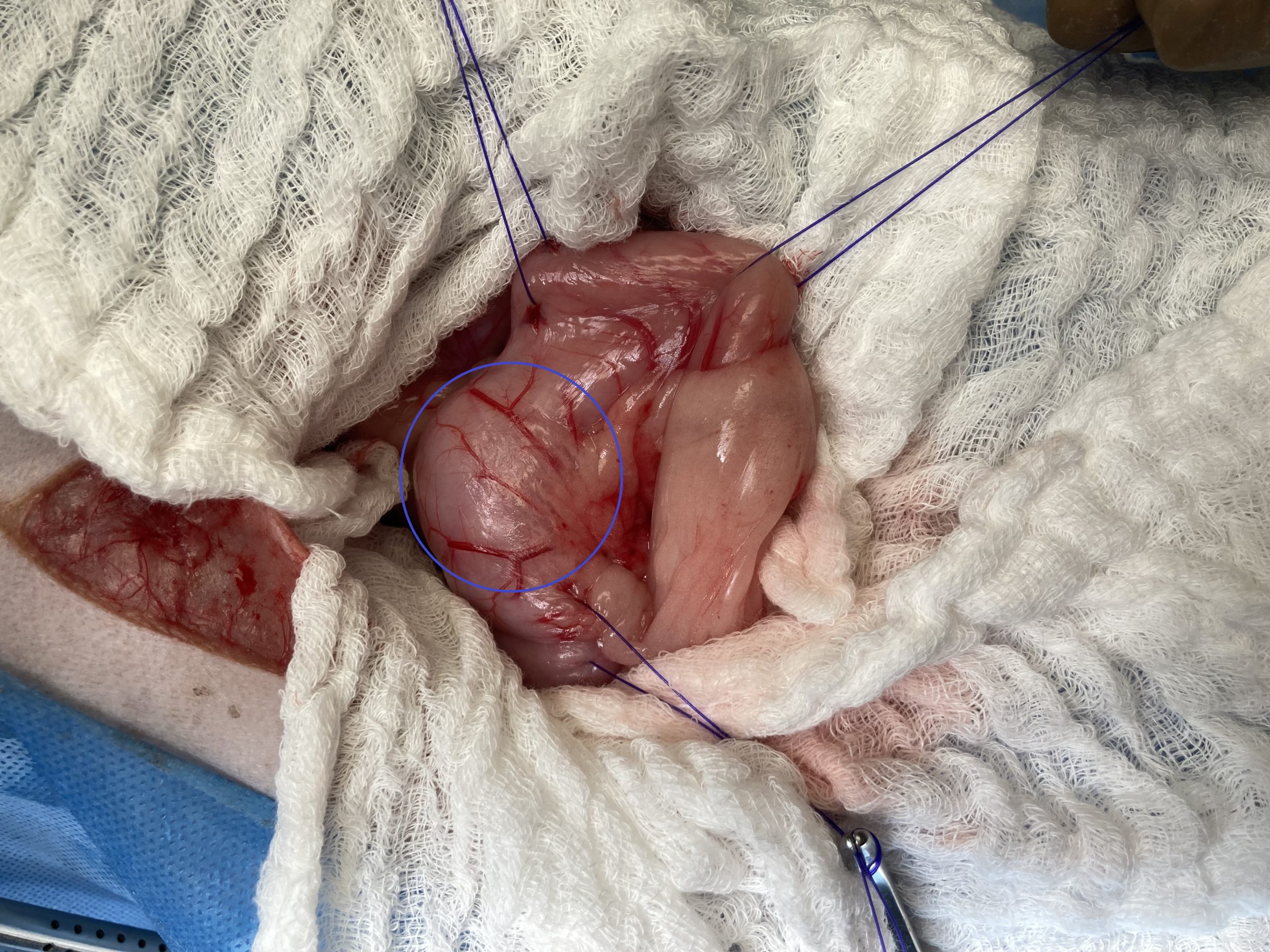
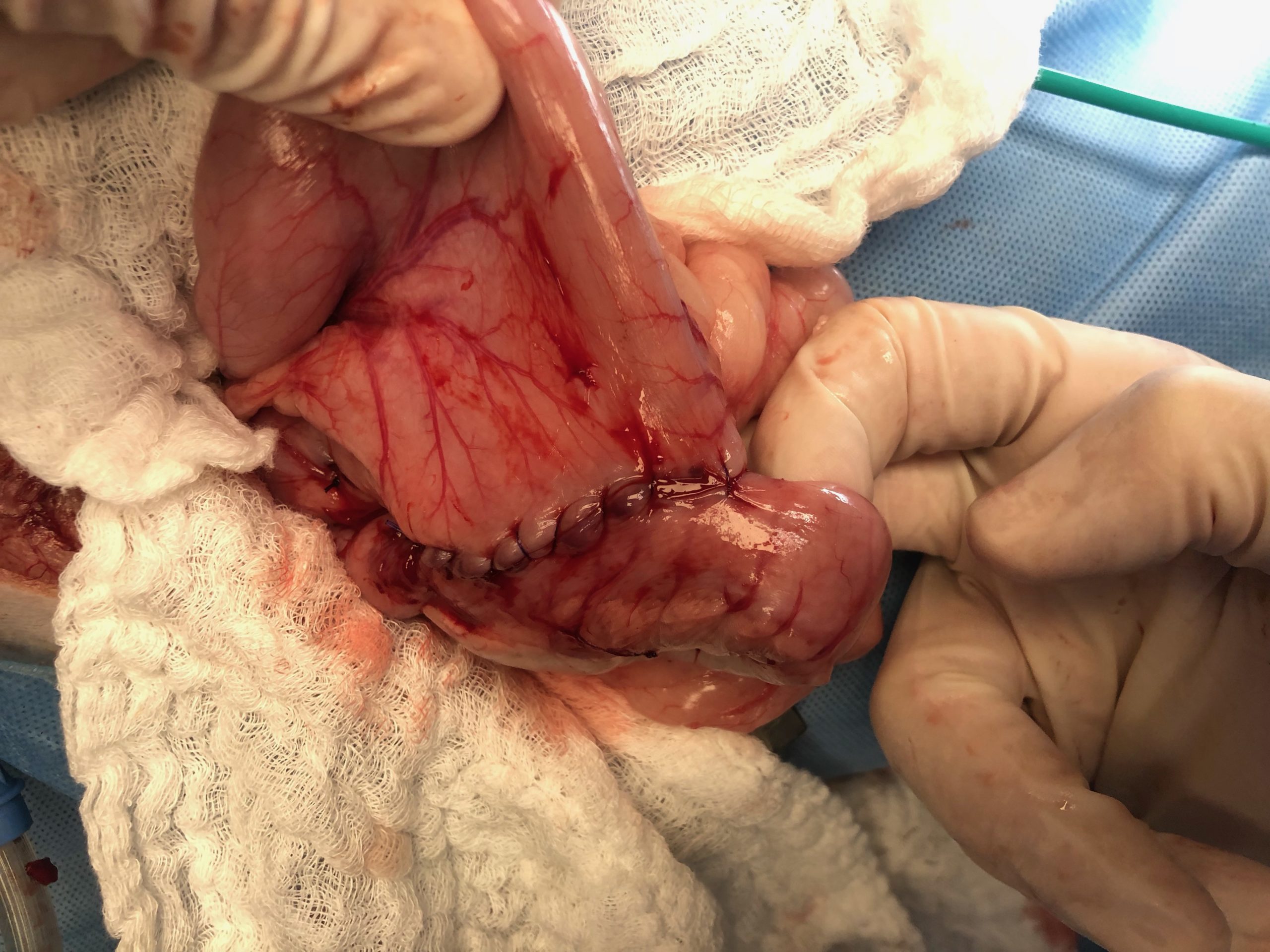
He generally had a poor appetite. He kept vomiting. He alternated between being lethargic and energetic. We tried different medications (more meds, fewer meds, new meds…). His incredibly dedicated owner tried multiple food types: regular kibble, new dog foods, baby food, people’s food (e.g., chicken breast), pureed food, food diluted with broth, several small meals. Nothing seemed to stop the vomiting or improve Max’s appetite. Of course, a poor appetite meant little to no poop coming out. He was mostly interested in drinking water.
It was an emotional rollercoaster. Should we give up? Did we do the right thing? His owner recalls: “We were scared. He looked so frail. He wouldn’t eat. He lost a lot of weight. I knew he was not happy. I was concerned he wasn’t going to recover, and we were going to need to put him down. We knew that this was major surgery, so it was difficult to see him this way.”
One week after surgery, the biopsy report came back. Unfortunately, a cancerous tumor of the muscle in the stomach was confirmed (leio-myo-sarcoma). Fortunately, it was “low grade,” which meant the tumor would not grow very quickly. Ironically, that didn’t matter. Benign or malignant, the mass would continue to grow and block the stomach. Then two weeks after surgery, like magic, Max turned the corner. His owner writes: “Just a quick update to let you know that Max is doing fantastic!” His appetite returned. His poop became normal. He showed an interest in his toys. Blood work showed that his red blood count doubled to a “high normal” level of 53% (it was 23% the day of surgery!). Of course, it’s still early. We know Max has cancer.
Still, his owner concludes: what matters “is not the age of the pet, but looking at the quality of life. I am so glad we were able to give him more time – more time to really live and to be happy with us.”
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified
www.HRVSS.com
Quick update 6 weeks after surgery
“Knock on wood, but I think I got his acid reflux under control and finally have most of his food issues resolved.
He is so spunky!
It’s like Max reverted back to his old self 5 years ago!
He barks at the vacuum cleaner, and chases Fozzee, our 3 year old Bernadoodle around the yard without missing a step!
He actually keeps up with him!
He still regurgitates once in a while but that has significantly decreased, and his bowel movements are perfect.
His stomach doesn’t gurgle nearly as much and he is putting on a little weight.
I understand his prognosis and know that we can’t really change it, but to see him – you would NEVER know he has (or had) any issues.
(…)
Just wanted to thank you for giving us this extra time with Max.
He is like Max 2.0, haha!”

